|
The likely causes of PEA in traumatic arrest are hypovolemia, tension pneumothorax, and cardiac tamponade if the hands can be redirected from chest compressions to a procedure that corrects an underlying cause, like airway management, IV/IO access and a fluid bolus, decompressing a pneumothorax, pericardiocentesis, or binding the pelvis, prioritize that instead of mashing the chest. The AHA recommends standard-practice CPR in cases of traumatic cardiac arrest, but offers no evidence that it works, and the survival rate from traumatic cardiac arrest is dismal. If they don’t, what a wonderful topic to research and present to your medical director, especially if the number of providers on scene is limited. If your protocols allow field termination or not starting CPR, follow your protocol. If it’s PEA from traumatic arrest, hold off on CPR If you’re not up to speed on the suspicious findings for coronary occlusions, hyperkalemia, or pulmonary embolism from a 12-lead ECG, get studying! 4. Before raising objections, hear me out you can still place the precordial electrodes appropriately (or very closely) while chest compressions are ongoing, and acquiring a 12-lead ECG only takes about 10 seconds, so there’s no need to pause high-quality CPR for longer than the AHA currently recommends.Īnd in cases where the likely cause of arrest is elusive, the information from a 12-lead ECG can help immensely. If there aren’t any big red flags pointing you towards any of the possible H and T causes, consider stopping CPR for enough time to acquire a 12-lead ECG. 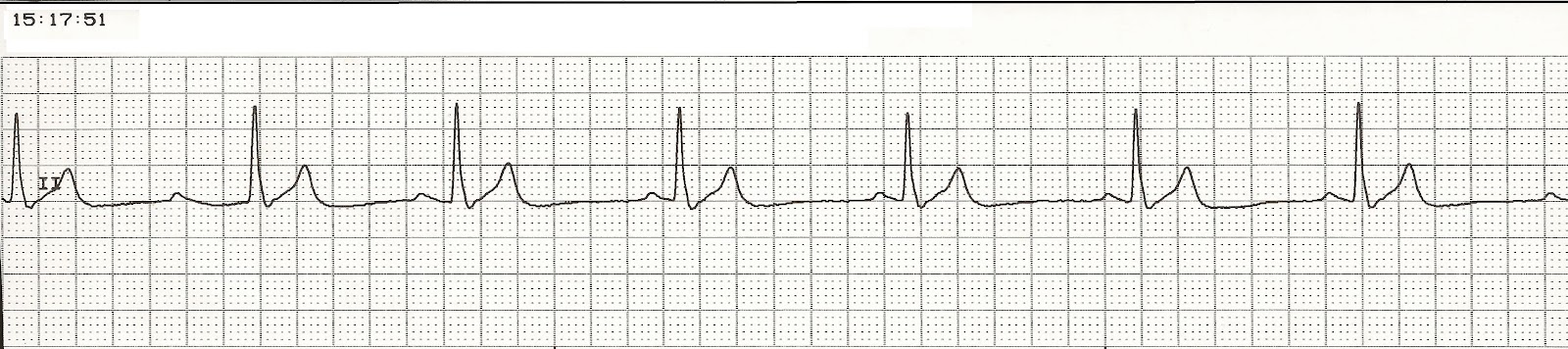
Are there risk factors for PE or hyperkalemia? Any scene indicators that an overdose might have occurred? Jugular venous distension or minimal chest rise that might suggest cardiac tamponade or tension pneumothorax? Paying attention to the characteristics of the ECG rhythm can narrow the field of possibilities some, but assessing the patient’s medical history and performing a quick physical exam are still crucial for identifying the cause of PEA. Wide QRS complexes typically indicate a metabolic problem (such as hyperkalemia or sodium-channel blockade from a toxic overdose), or left ventricular failure (either acute or chronic).Cardiac tamponade or a pulmonary embolism obstructs the right ventricle’s ability to pump blood to the pulmonary circulation and to the left atrium and ventricle. Problems like hypovolemia, tension pneumothorax, or hyperinflation of the lungs decrease inflow of blood into the right atrium and ventricle, reducing stroke volume and cardiac output. Narrow QRS complexes typically indicate an inflow or outflow problem with the right side of the heart.Littmann, Bustin, and Haley have a great article that explains this approach in detail. 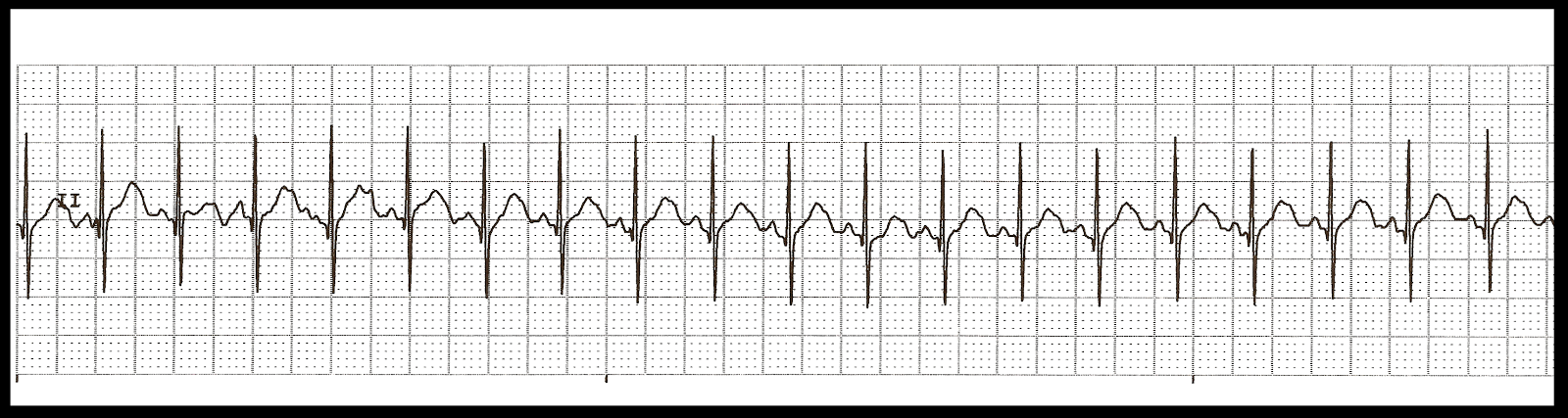
The ECG rhythm, or more specifically whether the QRS is narrow or wide, can give you some insight into likely reasons this patient arrested. The H’s and T’s mnemonic is a somewhat comprehensive listing of possible causes of PEA, but it doesn’t provide much in the way of guidance on which possible causes you should look into first. Why are we giving epinephrine to cardiac arrest patients?
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
